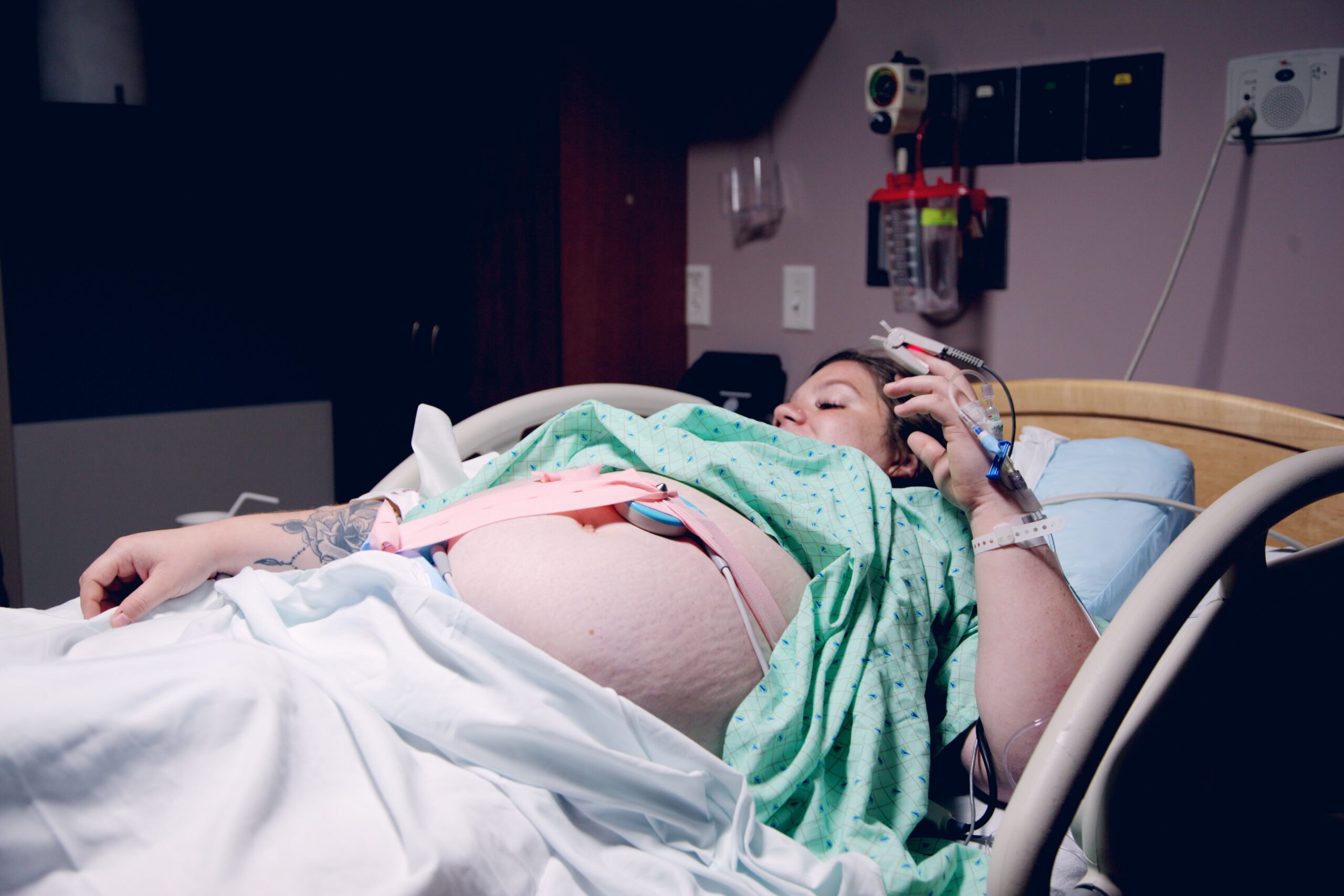
I hope that no other mother or baby is harmed in the same way that my baby and I were during labor and delivery. That’s why I’m sharing our story.
- Inflammation or infection of the fetal membranes (chorion and amnion) and the amniotic fluid surrounding the fetus
- Affects 1-4% of full-term deliveries (after 37 weeks) and 40-70% of premature births (before 37 weeks)
- Most commonly develops during labor and delivery, but can also occur before labor or in cases of prolonged rupture of membranes (when the amniotic sac breaks before the onset of labor)
- Occurs when bacteria from the mother’s vaginal or gastrointestinal tract ascend into the uterus, leading to infection
- Risk factors include longer duration of membrane rupture (more than 12 h), prolonged labor, nulliparity (not given birth before), internal monitoring of labor, multiple cervical exams, meconium-stained amniotic fluid
- Symptoms include maternal fever, increased maternal heart rate, uterine tenderness, foul-smelling amniotic fluid, maternal leukocytosis (an elevated white blood cell count), increased fetal heart rate
- Consequences can include preterm labor, sepsis (infection spreading throughout the body), postpartum infection, respiratory problems or brain damage for the newborn, stillbirth or neonatal death
I was classified high-risk when I became pregnant at the age of 41, yet I had a healthy pregnancy. I had planned on having a vaginal birth. I was aware of its advantages for babies. I’d read about how the mother’s vaginal microbiomes, which are passed on to the baby during birth, can aid to create the infant’s own gut microbiomes, enhancing later health (although this year, new evidence has disputed the concept that the mode of delivery matters). More than having a natural experience for myself, my mindset was that I wanted to give my baby the best possible start in life.
I’d taken a birthing class, read hypnobirthing books, watched childbirth videos on YouTube, and listened to other people’s birth stories. I was well aware that plans can change and that no matter what we want, we cannot control all of the outcomes in advance.
Having experienced a miscarriage, I knew intimately what pregnancy loss feels like.
The health and safety of my baby was always on my mind. I’d read about everything from choline’s relevance in brain development (I made sure I had extra choline throughout my pregnancy) to placental health in late-life pregnancies. I was aware of placental calcification, a deterioration process caused by tiny calcium deposits on the placenta. The placenta is an organ that helps the growing baby survive by transporting nutrients and oxygen and protecting the fetus from toxins, bacteria, and hormones. I was concerned since I was older, and some studies say that older mothers can have more issues with the placenta. This is a contentious topic, and many experts differ.
My friend had a stillbirth a few years before. It was weighing heavily on my mind. While there are numerous risk factors and causes of stillbirth, the autopsy revealed that her stillbirth was connected to the placental function. Her baby’s death was such a devastating experience. I knew what it was like to lose a pregnancy because I had had a miscarriage. I’d written an entire book of poems to navigate my grief. I couldn’t imagine the pain of losing a baby after nine months of bonding and waiting. I wanted my baby girl, who had become the most real to me since the 12-week scan when she was pictured smiling, to arrive alive and breathing in my arms.
I walked up the hills, drank raspberry leaf tea, and ate spicy food, but the baby didn’t budge by its due date. I even devoured eggplant parmesan that my poor partner, Ken, cooked all day according to a recipe from Scalini’s restaurant in Georgia, which is known to send women into labor within 48 hours—nothing happened. My OB and I discussed the possibility of induced labor. While many women are perfectly fine waiting until 41 weeks or when the baby is ready to come out, I was concerned about my age, the placenta failing, and a looming loss. I wanted to maximize the chances of a healthy outcome, so I agreed to the medical induction rather than waiting for labor to begin naturally. Trusting the medical process was the first decision I made.
I was scheduled for induction at 40+3 at 4 PM on a Wednesday in January in a downtown hospital. That very morning at 10 a.m., as I arose from the couch after stretching along the Miles Circuit, I felt a trickle of amniotic fluid (the Miles Circuit has been described as a natural induction technique, and I must admit it works). My waters had broken on the living room floor but there were no contractions. In medical terms, I was experiencing a spontaneous prelabor rupture of membranes (PROM) without the onset of labor. When I called the hospital for advice, I was told to come in right away because there was a risk of infection.
I got changed and packed my bag. When Ken and I arrived at the hospital at 11:45 a.m., I informed the Labor & Delivery unit’s front desk that I had called in earlier, was there to be induced, and that my waters had broken. In triage I was found to be grossly ruptured and nitrazine positive, confirming that I was leaking amniotic fluid.
Here’s what bothers me. Despite my ruptured membranes, which made me vulnerable to infection (as the front desk had warned me over the phone), the medical professionals allowed me to pursue a vaginal birth from Wednesday to Saturday. Chorioamnionitis developed as a result of my prolonged labor and the daily cervical exams, gradually infecting my uterus and placenta, my body’s lifelines to my baby. My blood pressure rose, and I developed preeclampsia shortly before giving birth.
My baby girl was born with pneumonia, a particularly severe case of meconium aspiration, persistent pulmonary hypertension (PPHN), and suspected sepsis. She was cyanotic, pink, and limp, with little respiratory effort, covered in meconium, and quiet. Her APGAR score was 2 at one minute, 6 at five minutes, and 7 at ten minutes of life. She couldn’t breathe on her own and needed immediate intubation, suctioning of the lungs and stomach, and invasive mechanical ventilation.
Separation from her mother was my daughter’s first experience in this world. She spent the first few weeks of her life in a baby incubator, receiving oxygen through a tube in her nose from a tank. This bed encased in clear hard plastic separated us for weeks. My daughter was being fed through an esophageal tube into her stomach. Her newborn body had become entangled in ECG probes, a pulse oximeter cuff, and temperature sensors. These wires hampered our physical connection and delayed my ability to fully hold her. My baby stayed in the neonatal intensive care unit for 18 days, with her dad and I by her side.
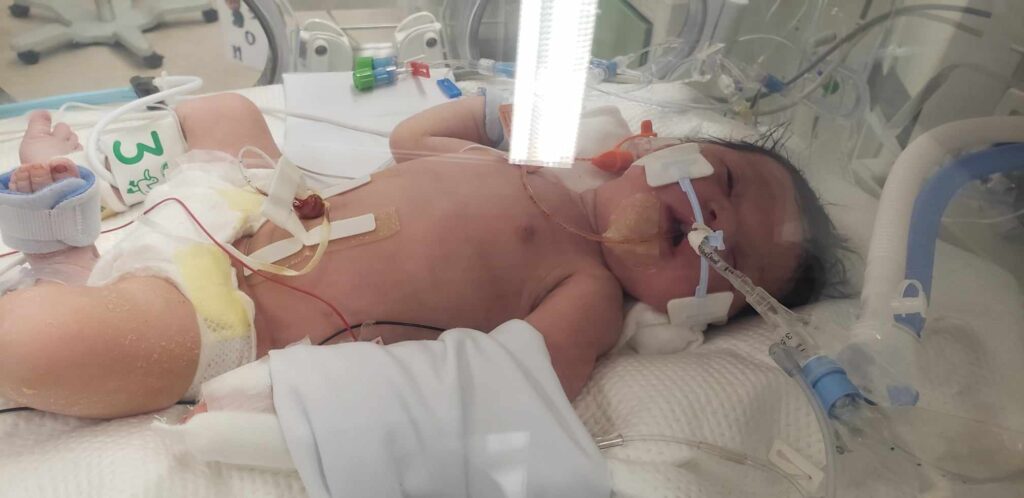
Several hospital events contributed to my baby’s birth in critical condition. I’ll explain these below.
1. Laboring with a prolonged rupture of membranes was unsafe for my baby
Since Wednesday (the day I was admitted to the labor and delivery unit), the obstetricians and midwives had been concerned about the slow progress of my labor. My cervix was not effacing and dilating as quickly as they had hoped. These same professionals also normalized a lengthy labor in the context of giving birth for the first-time. When being induced, it is common for things to move slowly.
I was given oral misoprostol for cervical ripening to soften, efface, and dilate the cervix and stimulate contractions. Misoprostol did not effectively ripen my cervix (as evidenced by the cervical exams listed below). It eventually caused such intense contractions that the breathing techniques I had learned in my hypnobirthing class were no longer effective. I had not anticipated such severe contractions and could no longer bear the agony.
The body may not be prepared for the rapid build-up of contractions when labor is induced. When the body is not prepared, it is unable to release endorphins to relieve pain as it is designed to do during natural labor. Natural labor is a more gradual process. All of the pressure from the induction medicines increases the risk of fetal distress because the baby is not prepared for such intensity.
On Thursday night, I was completely exhausted. I started talking about getting an epidural and eventually requested one around midnight. The epidural gave me a much-needed break, and I was able to sleep after being awake for 48 hours. Pitocin, a synthetic version of the hormone oxytocin, was introduced shortly after. Pitocin is used to either initiate contractions or to strengthen contractions that are too weak to allow cervical dilation and movement of the baby’s head down into the pelvis.
Despite having all of these medications in my system, the labor was slow. Yet the professionals provided constant reassurance: “Your baby looks good on the monitor.” This meant that the fetal monitoring strips that were tracking my baby’s heartbeat indicated she was not in distress. Such assurance gave me the confidence to continue. As a result, when the professionals brought up a c-section, I interpreted it as a matter of personal preference, specifically whether I was tired of laboring. I turned down the offer.
Around 02:30 a.m. on Saturday, a midwife and a doctor arrived at the bedside. They checked my cervix and found it to be only 5cm dilated. I had been in the hospital for three days. We discussed a c-section once more. They presented me with two options. Either have the c-section right away or wait 4 hours. I chose 4 more hours because I was told again that my baby looked good on the monitor. I also agreed to a c-section if no progress was made after 4 hours. I mentally prepared myself for the c-section.
This conversation was a turning point in both my labor and my health. A few hours later, signs of infection appeared. According to my medical records, I was diagnosed with chorioamnionitis around 6 a.m. on Saturday morning, after experiencing maternal tachycardia and a fever of 38.7C / 101.66F. Even at this point, the doctors had not named the infection to me. Nobody said anything about what chorioamnionitis does to my body and my baby. Instead, I was informed that I had “spiked a fever.” Antibiotics were started to treat the infection without my knowledge.
I was also found to be fully dilated two hours later. Everyone, including myself, seemed upbeat about the labor progress. I had finally reached 10 cm. The c-section we had discussed earlier was no longer mentioned. Soon I was instructed to start pushing.
I had to go back and read clinical literature to figure out how the professionals deviated from safe practice, leading the infection to develop in my body.
Consider how several risk factors made me especially vulnerable to chorioamnionitis:1
- My bag of waters (amniotic sac) broke long before I actually delivered
- I had a long labor
- I had internal fetal monitoring
- I got epidural anesthesia during labor
- This was my first pregnancy
- I had frequent cervical exams during labor
The literature consistently shows that the longer the time between the breaking of the water and the delivery of the baby, the greater the risk of infection. Women who give birth within 24 hours of their water breaking have a lower risk of infection. In comparison, my induction lasted 72 hours (65 hours until the first push on Saturday at 9 a.m.), which is significantly longer than the safe timeframe.
Research also confirms a strong link between the number of cervical exams and the risk of chorioamnionitis. Patients who receive cervical exams with prolonged rupture of membranes are in an increased risk with exams almost doubling the number of bacteria at the cervix.2,3
In the Term PROM study, the number of cervical exams received increased a patient’s risk of chorioamnionitis, with 7-8 exams leading to 3.8 times the odds of having the infection, and 8 or more exams leading to 5 times the odds of having the infection.4 According to other reports, even three cervical exams have been shown to increase the risk.5 I had seven cervical exams, the first in triage and the rest at each handover in the delivery room:
- Cervical exam Wednesday at 14:00 Cervical dilation 0 [0/50/-2]
- Cervical exam Thursday at 22:44 Cervical dilation 2.5 [2.5/90/-1]
- Cervical exam Friday at 06:25 Cervical dilation 3 [3/90/-1]
- Cervical exam Friday at 12:18 No change
- Cervical exam Friday at 17:30 Cervical dilation 4.5 [4.5/90/-1]
- Cervical exam Saturday at 02:30 Cervical dilation 5 [5/100/-1]
- Cervical exam Saturday at 08:00 Cervical dilation 10 [10/100/+1]
The professionals claimed that they would limit cervical exams with me. However, the seven exams significantly increased my risk of chorioamnionitis, and they must have been aware of this. I went along with the exams because I was told I was “failing to progress” and I wanted to put my trust in the professionals doing their jobs.
However, not a single professional informed me that each time they checked my cervix, the likelihood of infection drastically increased. No one explained how, despite their sterile gloves, the infection-causing bacteria would be pushed upward into the uterus, infecting the amniotic fluid and the placenta that were sustaining my baby’s life. The infection had only ever been mentioned by the obstetricians and midwives in vague terms like “potential for incremental risk.” Nobody had identified the infection as a threat that needed to be actively avoided.
2. Lack of information prevented me from making an informed decision about a c-section
Chorioamnionitis is not a trivial infection. However, no risks or consequences of chorioamnionitis were named or unpacked in ways that I could understand to jeopardize my baby’s safety.
I only found out later that the consequences of maternal chorioamnionitis to a newborn include pneumonia or meningitis, brain damage, or death.6 The baby has an increased chance of being born with a neurodevelopmental disorder, specifically cerebral palsy. 7,8
Why wasn’t anything done to prevent the infection?
Since my progress was slow, the medical professionals should have laid out the risks and consequences of chorioamnionitis within the first 24 hours of induced labor. They should have clearly advised me that a c-section, if done immediately, could prevent chorioamnionitis from developing.
The fact that the professionals did not perform a c-section within the appropriate timeframe contributed to me contracting this infection and my baby being born in critical condition.
Let me be clear:
My preference for vaginal birth was not absolute. I would not choose a vaginal birth at the expense of my baby’s health.
I would not have deferred a c-section if I had been educated about my baby’s safety, just as I did not decline medical induction of labor or the numerous cervical exams.
I stated twice that if no progress was made soon, I would proceed to a c-section.
I was never warned that pursuing labor was dangerous.
I was not informed that there could be serious consequences that would require my baby to be admitted to the NICU.
I was not informed of the potential neurological risks to her development.
When a c-section was suggested, it was presented as a personal preference rather than a life-saving option for my baby.
I was posed as the decision maker, but I didn’t have all of the information I needed to make an informed decision or comprehend the gravity of the situation.
The medical professionals failed to lay out the risks and consequences clearly and in plain language, for example:
The infection I was exposed to would contaminate my uterus and placenta, causing my baby to become very ill or suffer neurological damage in utero and end up in the NICU. This would also mean that baby and I would have to be separated immediately after birth, denying me the opportunity for skin-to-skin contact and breastfeeding, both of which I had prioritized in my birth plan.
This would have been crucial information for me to have.
Without relevant information about the risks and consequences, I was unable to make an informed decision and maximize my baby’s health. If I had known I was laboring in unsafe conditions, I would have elected to a c-section within the first 24 hours and most likely avoided the infection.
I was not oblivious to the risk of infection and mentioned it several times during labor. Nonetheless, the responses I received made me feel confident that it was safe to pursue a vaginal birth:
- On Wednesday (my first day in the hospital), I asked a midwife if my baby would run out of fluids because I was leaking. She said the amniotic fluid would replenish itself and didn’t seem concerned that I was leaking amniotic fluid.
- On Friday, I informed a nurse that my urine in the catheter bag appeared pink/red. I inquired as to whether this meant an infection. The nurse said she didn’t think so, and that catheter insertion can sometimes cause that. I felt reassured that it was not a sign of infection.
- On the same Friday, I asked a doctor at my bedside if she thought I had an infection. She, too, “did not think so.”
- “Your baby looks good on the monitor,” midwives and doctors said repeatedly. Their assessments about safety and wellbeing seemed to revolve around the fetal monitoring strips. The known risks to the baby associated with maternal chorioamnionitis to which I was exposed were not discussed.
The bottom line is that the medical professionals were clinically aware of the safety risks associated with chorioamnionitis in the context of a long labor and prolonged membrane rupture. As a result, I have found their care and communication to be injudicious, incautious, and negligent.
Please raise awareness about chorioamnionitis to protect moms and babies. Many hospitals are hesitant to admit if the infection was contracted while under their care, and many moms have been misled. Many more have been discharged from the hospital after leaking clear liquid. You may discover the infection through your medical records and discover that the medical professionals never informed you.
Keep an eye out for the following:
-
- Waters breaking. It isn’t always a gush or even obvious. It can be a trickle. Because ruptured membranes increase the risk of infection, it is critical to know if your water has broken. Get checked if you are unsure whether you have peed yourself or are leaking amniotic fluid. It’s better to be safe than sorry.
-
- If the hospital tries to discharge you without checking you with amniotic swabs, demand that they do so and inform them that you are aware of the infection risk. I sat in triage for two hours with no one checking my waters. Only after I reminded the triage nurse that I was leaking did she retrieve the amniotic fluid indicator swabs.
-
- Labor may not begin if your water breaks. You may not experience any contractions at all. This is what happened to me. Even if nothing appears to be happening, your birthing canals are open, exposing you to infection.
-
- You have the right to refuse cervical exams. After your water break, you are more likely to develop chorioamnionitis from any number of cervical exams.
-
- In labor, advocating for yourself is difficult. You may feel conflicted. It can be challenging to refuse cervical exams. Medical professionals often present the exams as necessary to determine how dilated and effaced you are, and where the baby’s head is (baby’s station) – information needed to work out when you might be ready to push. You may feel obligated to comply if you’ve had a long labor or have been told that you’re not progressing. You can inform the professionals that you are aware that cervical checks increase the risk of infection and that infection can harm your baby. It has the potential to change the entire conversation and the outcome.
-
- You may also be interested in the progress of your labor. Just keep in mind that the cervical exam only provides information in the present moment and cannot predict how quickly your cervix will change. The information you receive may provide you with false hope or discouragement. Hearing that you are not progressing can put your nervous system on high alert and cause your labor to stall: when we perceive a threat, even if it’s emotional or psychological, the body has the capacity to shut down the reproductive processes, including labor, in order to protect us. When labor stalls, it potentially exposes you to additional interventions.
-
- Fingers come in different sizes. A cervical exam may be incorrect because you are being measured by multiple people. My OB checked my cervix three days before my scheduled induction and found that I was 1 cm. The triage nurse claimed I was 0 on the day of my induction—her fingers were big and stubby.
Featured photo credit: Alexander Grey on Unsplash
References
1. Chorioamnionitis. Retrieved from Cedars-Sinai: https://www.cedars-sinai.org/health-library/diseases-and-conditions/c/chorioamnionitis.html
2. Slagle, H. B. G., Hoffman, M. K., Fonge, Y. N., Caplan, R., & Sciscione, A. C. (2022). Incremental risk of clinical chorioamnionitis associated with cervical examination. American Journal of Obstetrics & Gynecology MFM, 4(1), 100524.
3. Imseis, H. M., Trout, W. C., & Gabbe, S. G. (1999). The microbiologic effect of digital cervical examination. American Journal of Obstetrics and Gynecology, 180(3), 578-580.
4. Seaward P.G., Hannah M.E., Myhr T.L., Farine D., Ohlsson A., Wang E.E., Haque K., Weston J.A., Hewson S.A., Ohel G., & Hodnett E.D. (1997). International Multicentre Term Prelabor Rupture of Membranes Study: evaluation of predictors of clinical chorioamnionitis and postpartum fever in patients with prelabor rupture of membranes at term. American Journal of Obstetrics and Gynecology, 177(5), 1024-1029.
5. Tita, A. T., & Andrews, W. W. (2010). Diagnosis and management of clinical chorioamnionitis. Clinics in Perinatology, 37(2), 339-354.
6. Chorioamnionitis. Retrieved from Stanford Medicine Children’s Health: https://www.stanfordchildrens.org/en/topic/default?id=chorioamnionitis-90-P02441
7. Tsamantioti, E., Lisonkova, S., Muraca, G., Örtqvist, A. K., & Razaz, N. (2022). Chorioamnionitis and risk of long-term neurodevelopmental disorders in offspring: a population-based cohort study. American Journal of Obstetrics and Gynecology, 227(2), 287-e1.
8. Wu, Y. W., Escobar, G. J., Grether, J. K., Croen, L. A., Greene, J. D., & Newman, T. B. (2003). Chorioamnionitis and cerebral palsy in term and near-term infants. JAMA, 290(20), 2677-2684.